Last Updated on October 2, 2022 6:00 pm
BOONE, N.C. —A new study by a multidisciplinary team of researchers at Appalachian State University and the North Carolina Institute for Climate Studies (NCICS) indicates a significant association between COVID-19 transmission and humidity in some U.S. cities.
The study titled “Short-term effects of specific humidity and temperature on COVID-19 morbidity in select US cities,” was recently published in the journal Science of the Total Environment.
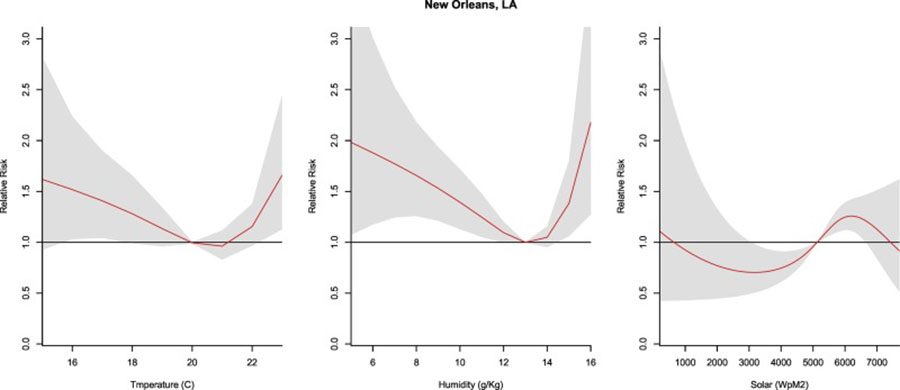
The authors wrote that, compared to solar radiation and temperature, the humidity was the most predominant predictor of COVID-19 transmission in U.S. cities considered among early hot spots in the pandemic.

Specifically, there was a higher risk of transmission in ranges of lower humidity and which resulted in as much as a two-fold increased risk of transmission in some areas. Early research in China and other international locations reported a similar relationship, according to the researchers.
“With respiratory viruses, humidity is often a main driver of transmission and we had hypothesized this may be the same for the coronavirus, which is a type of respiratory virus. Our results identified a significant relationship between COVID-19 transmission and humidity in three cities: Albany, Georgia, New Orleans and Chicago,” said author Dr. Maggie Sugg, an assistant professor in Appalachian State University’s Department of Geography and Planning who studies climate and health.
Other cities included in the study were Seattle, New York City, Detroit, Pittsfield, Massachusetts, and Bridgeport, Connecticut.
The study’s results may be helpful in informing public health interventions, the authors said.
“Our study is in many ways preliminary, but our results suggest that even though weather is secondary — there are behaviors such as handwashing, wearing a mask, adhering to social distancing guidance that are more important, weather is a factor. And, weather is a factor that is often omitted in infectious disease modeling,” said Dr. Jennifer Runkle, an environmental epidemiologist at NCICS and research assistant professor at Appalachian.
About the study


The researchers analyzed 266,760 cases and 19,729 deaths during a 40-50 day period across the cities in association with environmental factors, using data from the Johns Hopkins Center for Systems Science and Engineering repository, which continually assembles global COVID-19 cases, and meteorological data from the European Center for Median Range Weather Forecast (ECMWF) atmospheric reanalysis dataset. Results varied among the cities despite researchers’ accounting for social distancing measures.
Sugg said her group’s paper is the first published study in the U.S. using methods beyond simple correlation to examine weather parameters and COVID-19.
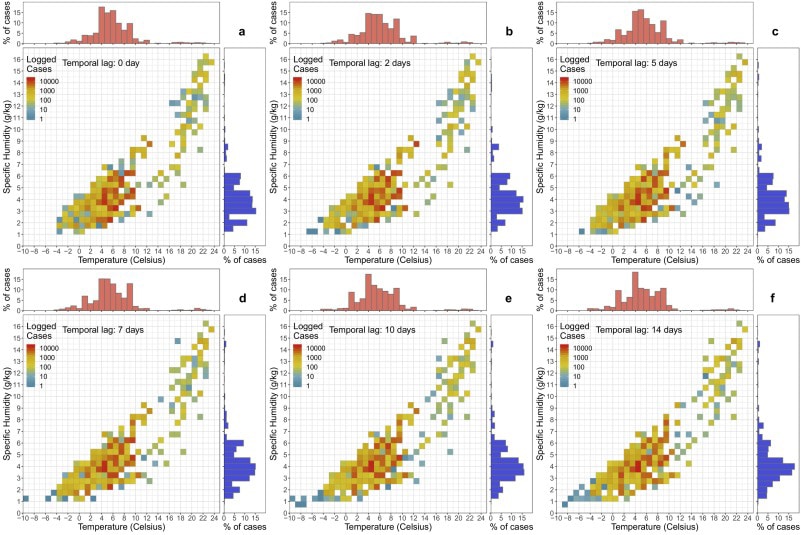
As an initial step, the authors generated density “heatmaps” that plotted daily cases across all eight cities against different combinations of daily air temperature and humidity for various lead times between the observed weather condition and the observed case count. These heatmaps suggested that COVID-19 cases were more common in conditions with low humidity (2–6 g/kg) and low temperature (35.6°– 51.8°F).
To explore these associations in more detail, the team then applied an innovative research design that used each person as their own control during a short window of exposure and allowed the researchers to measure the delayed effect of weather on COVID-19 transmission. The research design accounted for the presence or absence of social-distancing measures on a daily basis.
The authors wrote in the published paper, “Our results suggest that weather should be considered in infectious disease modeling efforts. Future work is needed over a longer time period and across different locations to clearly establish the weather-COVID19 relationship.”
Sugg and Runkle said they soon plan to expand the study to more cities and for longer timeframes.